Healthcare Revenue Cycle Management
A new Navigant analysis has found that over 60 percent of hospitals and health systems are not realizing optimal value from their EHR system.
Read MoreAn article at HealthcareDive.com paints a bleak picture for healthcare providers who are not staying up-to-date with the latest digital patient interfaces. About 41% of patients said they would consider switching providers for a better digital experience, according to a survey of more than 1,600 adults commissioned by New York-based patient billing company Cedar. Compared…
Read MoreYou might remember the post where we explored the misadventures of a patient who tried — in vain — to anticipate and control the costs of a planned procedure by interacting with his medical facility. It didn’t go so well. Loyale Healthcare recently asked a question that a lot of people — medical professionals and…
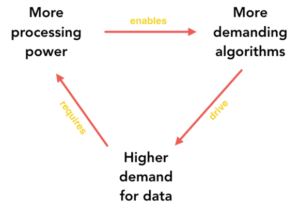
Read MoreMoore’s Law famously states that the number of transistors on a microchip doubles every two years, though the cost of computers is halved. A new essay on Medium.com explores how Moore’s Law had actually been “phasing out” for a period of time: Moore’s Law, one of the fundamental laws indicating the exponential progress in the…
Read MoreThe Office of the National Coordinator for Health IT’s (ONC’s) has issued guidelines for adopting application programming interfaces (APIs) into health data and EHR use. (You can see their report on hospitals’ usage of EHR data here.) The organizations who signed on to the letter are: American Academy of Family Physicians American Academy of Neurology…
Read MoreModern insurance plans — and, indeed, cases where people remain un- or under-insured — mean that whenever possible, healthcare consumers want to be able to anticipate potential costs as accurately as possible. This is the dawn of “retail healthcare” when it comes to certain anticipated, nonemergency cases, and consumers have a growing array of resources…
Read MoreAt the The 2019 OPEN MINDS Management Best Practices conference, Senior Associate Ken Carr provided a deep dive into that subject in his session entitled Are You Ready For Value-Based Reimbursement? An Executive Guide For Assessing Readiness In A Value-Based Market, which is summarized at the Open Minds website. During the session, Mr. Carr zeroed…
Read MoreBecker’s Hospital Review has looked over some recent studies and surveys to create a short and sweet list of insights regarding Artificial Intelligence and its role in transforming the Revenue Cycle Management process. The magic spot is the intersection between overcoming costs and creating a better, more effective patient experience. Yes, artificial intelligence implementation helps…
Read MoreAs reported at McKinsey.com, an analysis by the McKinsey Global Institute (covering more than 800 jobs and over 2,000 work activities) showed that: Globally, almost half the activities employees perform—which account for nearly USD 16 trillion in wages—could potentially be automated using existing proven technologies. Automation will transform far more jobs than it will eliminate.…
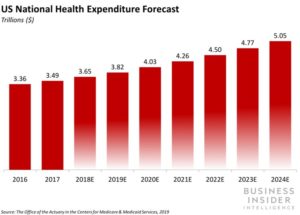
Read MoreThe US healthcare payments market is gigantic, and getting bigger. As seen in the chart above, Healthcare expenditure hit $3.65 trillion in 2018 (per projections from CMS) and this spending is only expected to go up and up (again, as seen in the ski-jump above). Does that mean cruise control for players in the healthcare…
Read More